Aimee Boyd MCPara, Research Co-Ordinator, Paramedic, Yorkshire Ambulance Service
I was still a newly qualified paramedic when I decided to participate in the BREATHE research trial. BREATHE is a study investigating
Breathlessness RElief AT Home. It’s working off the statistic that 1/3 of the people living with chronic respiratory diseases (such as Chronic Obstructive Pulmonary Disease (COPD)) and breathlessness who are taken to hospital, are discharged with no additional interventions. The long-term aim of the BREATHE study is to see if this breathlessness management intervention is effective at increasing safe on scene discharges in this patient demographic, rather than taking them to the ED when not needed. This part of the study was a feasibility trial; it’s a smaller scale of the study to see if it is possible and acceptable for paramedics on the road to collect consent and data from breathless patients and carry out the intervention, before a full study takes place on a larger scale to see if the intervention is effective.
I initially signed up because I wanted to get some training and CPD under my belt. I also knew research is one of the College of Paramedics ‘Four Pillars.’
What I didn’t count on, was a respiratory virus interfering with things!
I completed training for the study around May 2020 – so we were still in our first COVID lockdown. I don’t think training for BREATHE paramedics was initially planned to be held online, and I hadn’t participated in anything virtually before. I think there are positives and negatives to online training – I didn’t have to commute anywhere and we still had our cameras on, so we were given some feedback about the techniques we were using. It would have been nice to do it in person so I could practice coaching another person through the techniques, rather than modelling them myself.
I was in the intervention arm, so I had some additional training on the BREATHE intervention. We used the BREATHE acronym, as both an aide memoire and a training tool, to help patients and their carers manage breathlessness independently. BREATHE stands for;
- Be reassured
- Resting positions – get comfortable, relax your shoulders
- Exercises to calm your breathing
- Airflow – using a fan, or opening windows
- Take your time
- Help with fears, use an action plan
- Educate – read the booklets for practical solutions to help.
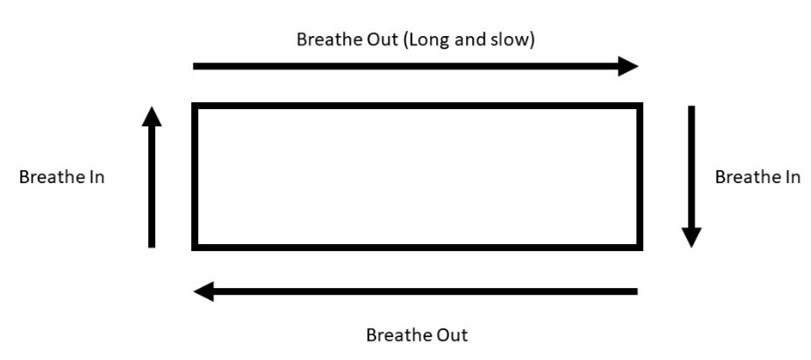
We were given fans to give to each patient, but we were unable to use them due to the unknown risks of COVID at the time. This was a shame, because when I have been to COPD patients in the past, I know they found fans helpful. Outside of the trial, I would give patients a folder paper fan. We did some breathing techniques where the patient looks at a window or a TV screen – anything rectangular, and focuses on breathing out on the long edges, and in on the shorter edges. This helps prevent short sharp hypoventilations that can make a person feel like they aren’t getting enough air, and the anxious feelings that follow. This is so easy and relatives would always take over coaching without any prompting from us as the crew. Finally, to help people relax, we put pillows under their armpits – it really works! People are suddenly aware of how much tension they are holding in their shoulders.
We also asked patients to rate their breathlessness every few minutes, on a scale of 0-10, where 10 is extremely breathless, and 0 is not breathless at all. It’s a good tool for patients, because they can see from their own self report that their breathlessness has improved compared to their baseline. For me, it was helpful to document something quantitative to reiterate breathlessness had improved.
Despite the inclusion and exclusion criteria being clear, it was tricky to recruit patients as I didn’t know where we stood with COVID patients. I would be really interested to see how COVID and long COVID are built into the inclusion and exclusion criteria should we do further research with BREATHE. Even though I didn’t recruit many patients into the trial, I found the techniques I learned worked well with patients having panic attacks, so it was nice to be able to apply that learning elsewhere in my clinical practice.
I really like that Ann, the lead researcher, is proactive about dissemination. Ann was keen to hear from us and she invited the recruiting paramedics to share our feedback, and I do feel like my feedback was valuable to them and will be something that is acted upon. I have also attended a conference where I have seen Ann present the study.
BREATHE was a great introduction to research in the pre-hospital environment for me!
Want to find out more?
For more information on the BREATHE study watch
this video.
Read the Protocol Paper - Northgraves M, Cohen J, Allgar V, et al. A feasibility cluster randomised controlled trial of a paramedic-administered breathlessness management intervention for acute-on-chronic breathlessness (BREATHE): Study protocol. ERJ Open Res 2021; in press (
https://doi.org/10.1183/23120541.00955-2020).
Read the Paper - Hutchinson A, Allgar V, Cohen J, Currow D, Griffin S, Hart S, Hird K, Hodge A, Mason S, Northgraves M, Reeve J, Swan F, Johnson M. Mixed-methods feasibility cluster randomised controlled trial of a paramedic-administered breathlessness management intervention for acute-on-chronic breathlessness (BREATHE): Study findings. ERJ Open Res, 2022. Doi:10.1183/23120541.00257-2022
Follow us on Twitter! - @YASResearch @AHutchinsonHull @HullYorkMed @wolfsonpallcare
https://www.hyms.ac.uk/research/research-centres-and-groups/wolfson/breathe
Find out more about getting into research
To find out more about getting into research,
click here to sign-up to the Research Drop-in Clinic, which takes place on Thursday 9th February 2023.